Craig D. Clayton and Dr. Jonathan Wisco, Physiology and Developmental Biology
The floor of the oral cavity is covered by a mucosal layer to protect underlying structures against the digestive events of the mouth. Ducts of the salivary glands open into this mucosa along the lingual frenulum. The lingual nerve from the mandibular division of the trigeminal nerve immediately begins to branch after passing through the foramen ovale, and continues its descent medial to the inferior alveolar nerve. Just superior to the angle of the mandible, the nerve turns anteriorly 90 degrees and continues a lateral to medial path to the anterior of the mouth. It crosses the submandibular salivary duct inferiorly, and becomes more superficial as it reaches the anterior portion of the tongue. This nerve sends branches into the posterior, inferior portion of the sublingual salivary gland, and to various locations in the lateral parts of the tongue. An anatomical literature search of conventional atlases of human anatomy revealed that descriptions of lingual nerve innervation of the gingival are absent, with the exception of Gray’s Anatomy, which teaches that the lingual gingiva in some cases receive innervation from branches of the lingual nerve (Gray’s Anatomy edited by Peter L. Williams)i. Henry Gray, however, does not include a verbal or visual description of these branches, i.e. the location, nerve course, and whether they pass through the sublingual salivary gland or not. The distinct characteristic found in my first dissection was the passing of lingual nerve fibers through the sublingual salivary gland before entering the gingiva.
A careful dissection of the oral cavity floor exposed small lingual nerve branches coursing between the sublingual salivary gland and the medial border of the mandibular gingiva, as described by Henry Gray. Twenty-nine dissections of hemisected human specimens were performed to explore the variance and probability of the existence and location of these branches in humans. These lingual nerve branches were classified by total number per specimen as well as by the gingival territory that they innervated, using the teeth as the landmark.
The oral cavity floors of 29 hemi-sected, human specimens were dissected to expose the individual lingual nerve branches. An incision was made 12.7mm from the medial border of the alveolar margin with a scalpel. Delicately, using hemostatic forceps and a reverse scissoring technique, the oral mucosa between the tongue and mandibular alveolar margin was removed to expose the underlying sublingual salivary gland, lingual nerve, submandibular salivary duct, and vasculature. Connective tissue strands were removed, isolating the lingual nerve and its branches. We delineated, but preserved, the location and spatial relationships between the lingual nerve, sublingual gland, and submandibular duct. Muscle and fascia were removed from the exterior and inferior surfaces, condylar process, coronoid process, and ramus of each mandible using a scalpel and scissors to aid in the modeling process described below.
The MicroScribe 3DX digitizer was used to digitize the specimens and create a three-dimensional (3D) model of the specimens. Three shallow holes were drilled into the body of the mandible, using a 3/16 inch drill bit and cordless drill, to serve as reference points for the MicroScribe 3DX digitizer. A ¼ inch hole was also drilled in the ramus of the mandible for the purpose of securing each specimen to a custom built wooden stand (using a 2 ¼ inch bolts and wingnuts) to restrict the movement of the specimen while it was digitized. Spatial data points of the mandible, tongue, sublingual salivary gland, submandibular salivary duct, lingual nerve, teeth, gingival, and lingual nerve branches were recorded using the MicroScribe tool.
The three reference points mentioned in the above step are used to calibrate the digitizing software and tool and thus create a spatial relationship between these fixed points and all additional data points recorded. A separate layer of data points was created for each structure digitized in order to organize the data as well as hide already recorded layers from view which helped to decrease the risk of error and confusion. The final product of the digitized data points is a 3D model of these points as they relate to one another (see image 1b). Upon completion of the data collection for each specimen, the point model was uploaded to Maya Autodesk to create a more realistic rendering of the structure.
The surface rendering software Rhino 3D is currently being used to create realistic properties such as surfaces, color, texture, and shape out of the point models created with the MicroScribe. These models will permit the viewer to rotate them in space in any direction to achieve a better understanding of the spatial relationship of these small branches with their surrounding structures.
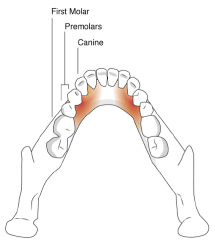
Of 29 specimens dissected, eighteen contained lingual nerve branches, emanating only from the anterior third of the lingual gland, which innervated either the territory of the incisor, premolars or first molar area of the gingiva regardless of the number of branches. Six specimens had one nerve branch between the sublingual salivary gland and gingiva, eight had two branches, and five had three branches.
As stated above, these nerve branches have, to our knowledge and research, have been classified but once in clinical anatomy literature. Being very small in nature, these nerves may be cut depending on the dissection technique used; for example, Grant’s Dissection Guide instructs the student to carefully incise the mucosa along the medial border of the mandible and then to carefully reflect back the mucosa, but medical and dental dissections often focus on identifying specific major structures within the floor of the oral cavity which could lead to the accidental removal or failed observation of these nerve branches. Dr. Wisco has concluded that the current dissection techniques used in many medical schools do not allow for the observation of these delicate nerves due to a rudely invasive technique employed only to see the large structures of the oral cavity. The introduction of our new dissection pedagogy to the scientific and clinical community can allow for the further exploration as to the variance, prevalence, and clinical significance of our discovery.
Currently it is not known whether these nerves are somatic or visceral and the function they serve also remains unknown. Will they be important in surgical settings or in the improved application of anesthesia for people who don’t respond well to typical procedures? We hop to address these questions in additional studies as well as to receive interest from the clinical community in solving and expanding upon this finding.
Figure 1-Partially constructed model. Includes surfaced model and microscribe point mesh
Figure 2-Heat map of the different regions of gingival innervation by the lingual nerve branches
i Gray, H. (1989). Gray’s anatomy (37th ed.) (P. Williams, Ed., et. al.). Edinburgh: C. Livingstone.