Michael J. Larson and Dr. Ramona O. Hopkins, Psychology
Each year thousands of patients become critically ill and require medical treatment in the intensive care unit (ICU). Recent literature suggests that patients recovering from critical illness have little or no recollection of their time in the ICU (1). The ICU has many features that may cause patients to become confused including isolation, sleep deprivation, and being surrounded with machines, lights, and constant noise (2). Sedative and analgesic drugs, mechanical ventilation, pain, and discomfort may also adversely affect ICU patients’ formation of memories (1).
Studies of patients’ memory of the ICU have measured patients’ direct recall of ICU events and/or procedures. Memory, however, is not a single entity but at least two separate entities that depend on different brain systems. The key distinction between the different types of memory is whether there is a capacity for conscious recollection of facts and events (explicit memory) or a heterogeneous collection of non-conscious learning capacities (implicit memory) (3). Studies of implicit memory are often conducted on amnesic patients. Several tasks (e.g., artificial grammar learning and mirror tracing tasks) can be performed normally by amnesic patients who do not remember training (4). Implicitly recalled events could also be manifest as dreams or hallucinations. Critically ill patients may implicitly remember events and procedures that occurred in the ICU that are not explicitly recalled.
In order to examine implicit and explicit memory of the ICU we interviewed 73 consecutive patients with acute respiratory distress syndrome (ARDS). ARDS is characterized by severe lung injury and profound arterial hypoxemia. ARDS occurs in response to direct or indirect insults to the lungs and is accompanied by multiple organ dysfunction and a high mortality rate. The purpose of our study was to assess explicit and implicit recollections of the ICU experience in ARDS patients.
Methods
Medical data and patient interviews were obtained from patients treated in Shock Trauma Intermountain Respiratory Intensive Care Unit just prior to discharge from LDS Hospital. The institutional review board at LDS Hospital approved the study and informed consent was obtained for all study participants.
Seventy-three ARDS patients were included in this study, with 33 males and 40 females. The mean age was 47.3 + 16.5 years (range 16 to 82 years). Patients’ interviews were conducted just prior to hospital discharge. The interviews were tape recorded, transcribed, and then coded for the number and type of events. Interviews elicited information on: 1) patients’ explicit memories of the ICU experience, including ability to move and ability to speak, and 2) dreams and/or hallucinations remembered while in the ICU. Descriptive statistics were calculated for patients’ explicit and implicit memories. Chi-square analysis was used to compare explicit and implicit memories (i.e., explicitly recalled memories of being unable to move to being unable to move in a dream).
Results
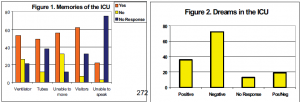
Patients’ explicit memories of the ICU are reported in Figure 1. Dreams were reported by 53 of the ARDS patients (73%) (Figure 2). Dreams were described as vivid with patients stating that they often thought the dreams were real. Of the 53 patients who reported dreams 40% reported being unable to move in their dreams, 34% remembered water and thirst in their dreams, and 6% remembered not being able to speak in their dreams. Chi-square analysis revealed no significant associations between explicitly recalling being unable to move and being unable to move in dreams (χ2 = .447, df = 1, p = .504), and explicitly recalling not being able to speak and not being able to speak in dreams (χ2 = .443, df = 1, p = .506). In other words, ARDS patients who could explicitly recall being unable to move or unable to speak were no more likely to have dreams about being unable to move or unable to speak than were other ARDS patients.
Discussion
Our study found that ARDS patients could explicitly recall events and procedures that occurred during the ICU. Sedative and analgesic drugs that patients receive in the ICU did not prevent memory formation. Many of the patients recalled dreams and hallucinations in great detail. Patients’ implicit recall of ICU procedures and events was not statistically significant; however, a large percentage of patients implicitly recalled being unable to move and feelings of thirst. Future research on patients’ memories of the ICU could lead to improvement of patient care through increased awareness of ICU caregivers.
References
- Jones, C., Griffiths, R.D., & Humphris, G. (2000). Disturbed memory and amnesia related to intensive care. Memory, 8, 79-94.
- Turner, J.S., Briggs, S.J., Springhorn, H.E., & Potgeiter, P.D. (1990). Patients’ recollections of the ICU experience. Critical Care Medicine, 18, 966-968.
- Squire, L.R., & Zola, S.M. (1996). Structure and function of declarative and nondeclarative memory systems. Proceedings of the National Academy of Science, 93, 13515-13522.
- Reber, P.J., Knowlton, B.J., & Squire, L.R. (1996). Dissociable properties of memory systems. Behavioral Neuroscience, 110, 861-871.