Angeline Abdo and Dr. Patricia Ravert, Nursing
Abstract
Background: Patient simulators are used in some nursing schools to simulate patient scenarios.
Methods: Nursing students participated in five sessions using the simulator and completed a student perception instrument.
Results: Participants felt the experiences recreated real-life situations and then tested clinical decision-making. The results indicated an increase in their confidence when going into the real clinical setting and the experience prepared them for the “real-life” clinical setting.
Conclusions: Overall patient simulator experiences enhance learning. Further research regarding student perceptions and instrument validation would contribute to an understanding of the use of patient simulators in nursing education.
Key Point Statements
Respondents were very positive regarding the transferability, realism and value of the simulation experience.
The human patient simulator appears to benefit students in their decision making skills, technical skills, level of confidence, preparation for “real-life” settings and in reinforcing the learning occurring in class.
More research regarding student perceptions and instrument validation is recommended.
Key Words
human patient simulator, patient simulator, nursing education, student perceptions, simulation education, student satisfaction
Student Satisfaction with Simulation Experiences
Nursing students have much to learn during their educational experiences regarding how to care for patients. Many student experiences depend on the kinds of patients on the units during their clinical rotations. Currently patient simulators are beginning to be used in some nursing programs. Patient simulators are computer-driven high-fidelity manikins which can be programmed to simulate physiological changes in the cardiovascular, pulmonary, metabolic and neurological systems with changeable heart and breath sounds, and chest movement. They allow students to administer simulated medications with appropriate physiological effects. The simulator can also be programmed to physiologically respond like a real person responds with a similar condition or disease, such as a decrease in blood pressure and increased heart rate with hemorrhage or shock. By using a patient simulator, instructors can provide students with a wide variety of patient problems and ensure they have an opportunity to learn the appropriate care. The patient simulator experience along with clinical practice experiences can give the students an appropriate background for their nursing career. In the past the patient simulators have been used extensively for training in anesthesia schools and now some undergraduate programs augment learning experiences gained in hospitals with simulation experiences (Bearnson and Wiker, 2005). Since hospitals expect more advanced skills in graduate nurses due to the increase in patient acuity and technology, the patient simulation experiences allow the practice of these skills (Feingold, Calaluce and Kallen, 2004). However, little research has documented use of patient simulation in nursing programs and especially student perceptions of the patient simulation experiences. Therefore, the purpose of this pilot study was to evaluate student perceptions of patient simulator experiences during their medical surgical nursing course. Hypotheses were, 1) students will rate the patient simulator experience as realistic and valuable with skills transferring smoothly into clinical situations, 2) students will feel more confident in their nursing skills, 3) students will feel more comfortable in clinical settings, 4) students will have a deeper understanding of the role of nurses, 5) and students will gain a truer clinical understanding of the situations they encountered in the simulation experience lab.
A college of nursing at a large private intermountain west university acquired a human patient simulator (HPS) manufactured by Medical Educational Technologies Incorporated. Since then the simulator has been incorporated on a routine basis into the curriculum. This project investigated perceptions of second semester nursing students regarding their experience with the HPS.
Literature Review
Patient simulators are being used in nursing education programs at a variety of levels (Nehring & Lashley, 2004). Benefits for students involved in simulation experiences are learning in a risk-free environment, being able to experience interactive learning, having the opportunity to practice skills, and receiving feedback immediately from a faculty member or tutor (Haskvitz, & Koop, 2004; McCartney, 2005; Morton, 1997; Nehring, Ellis, & Lashley, 2001). Another advantage is that the same patient problem can be presented to a number of students without risk to actual patients, and if necessary the simulation can be stopped for discussion or to replay the scenario (Feingold, Calaluce, & Kallen, 2004; Nehring, Ellis, & Lashley, 2001). Patient simulators can also be used to prepare students to manage medical emergencies (Spunt, Foster, & Adams, 2004). Finally, Nehring and Lashley (2004) believe using patient simulators gives professors the opportunity to teach important nursing management skills and suggests schools establish the validity and reliability of scenarios used with the patient simulator.
Few quantitative studies have investigated patient simulator experiences with nursing students (Ravert, 2002). However, Bearnson and Wiker (2005) found increased student knowledge, ability and confidence in medication administration when having experience with the HPS. In addition, Peteani (2004) found students show more autonomy and self-confidence after sessions with the patient simulator when compared to students who do not have the experience. Finally, a student satisfaction survey, developed through literature review to determine important aspects of simulation, reported nursing students found the simulations were realistic and valuable (Feingold, Calaluce, & Kallen, 2004).
Sample and Method
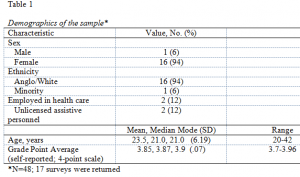
All 48 baccalaureate students in the first medical-surgical nursing course which used the patient simulator in a lab setting were invited to participate in the study. At the beginning of the semester, the research project was explained to the students. They were informed that their decision to participate or not participate in the study would have no impact on their grade. After the fifth simulator session the students who agreed to participate were given the opportunity to complete the student satisfaction survey. Of the 48 students, 17 responded to the student satisfaction survey. Complete demographics data are reported in Table 1. The sample was nearly all anglo/white females with an average age of 23.5 years. The self-reported grade point average was 3.8 on a 4-point grade scale. All participants surveyed had one semester of nursing school and one also had previous experience using the patient simulator. Two participants were employed in the health care setting as unlicensed assisted personnel.
Students attended five, one-hour sessions with the patient simulator. There were four students per session, as well as one registered nurse who facilitated and guided the session, and a research assistant who advanced the scenario and role-played the patient and medical personnel. During the sessions, the room and the patient simulator were set-up to be as realistic as possible, by presenting patients with congestive heart failure, myocardial infarction, traumatic brain injury, diabetic ketoacidosis, and gastro-intestinal bleeding. Students were given information regarding the scenario they would be working on two weeks in advance, giving them time to prepare and read about the condition before they actually experienced it. When students arrived for their session they received a nurses’ report about the patient’s condition and chose a team leader who divided up the tasks among the students. The team leader was given the patient’s chart and as a team, the students used the nursing process to care for the patient; assessing, diagnosing, planning and delivering for nursing interventions, evaluating and revising the plan as needed. The students were able to view the cardiac monitor showing the heart rate, blood pressure and respiratory rate, as well as the temperature and oxygen saturation. They were also given a chart which contained the health care provider’s orders and the patient’s lab values. Students were able to assess breath and heart sounds, respiratory rate, and peripheral pulses as well as start intravenous catheters and administer intravenous fluids, give medications, suction, check the urinary catheter, and insert nasogastric tubes.
As they went through the scenario the students talked to the patient and interacted with medical staff as they cared for their patient. During the session, the registered nurse asked thought provoking questions, lead the discussion, and answered questions. The teaching assistant role played the patient’s response as well as other heath care team members’ responses as appropriate to the scenario. At the end of the session, students were debriefed regarding what happened, what was done well and what could have been done better.
After the students completed the five sessions, those agreeing to participate in the study signed a consent form and completed the research instrument to analyze their perceptions. The data were entered into a statistical software program. Reliability estimates for the instrument and descriptive statistical analysis including means and frequencies were calculated.
Instrument
A 19-item student satisfaction survey, developed by Feingold, Calaluce, and Kallen (2004) used a 4-point Likert scale (1= Strongly Disagree, 2= Disagree, 3= Agree, and 4= Strongly Agree) to determine the extent the participants agree with the items. The instrument has three subscales: realism (n=3), transferability (n=3), and value (n=6). The survey investigated the students’ perceptions of the reality of the scenario with an item such as “The scenario used with the patient simulator recreates real-life situations.” The transferability of the scenario to clinical situations was assessed with an item such as “My interaction with the patient simulator improved my clinical competence.” The value of the patient simulator to their learning was assessed with items such as “Overall the simulator experience enhanced my learning.” The reliability estimates in prior use were not reported. The survey included additional individual items (n=7) related to the patient simulation experience.
Results
The reliability of the overall student satisfaction instrument for this sample showed .86 for the coefficient alpha. The reliability of the purposed subscales for this sample showed coefficient alphas of .41 for realism, .78 for transferability, and .69 for value. Initial factor analysis was run and showed between 3-6 subscales per scree plot and eigenvalues >1. Even though the overall alpha was .86, the underlying subscales had low alphas which may indicate too few items or subscales were not purposed correctly given the initial factor analysis.
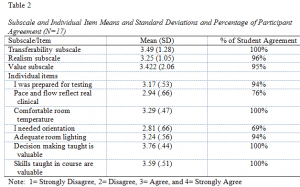
The results from the survey were analyzed according to the original subscales of transferability, realism, and value. Means and standard deviations for all variables were computed (see Table 2). The transferability subscale (3 items) showed all students agreed with the survey items regarding transferability, or the ability of the things done or learned in the sessions to transfer to the clinical setting. A majority of the students agreed the scenario reflected real-life situations, settings and patients as reflected in the realism subscale (3 items). The value subscale (6 items) grouped together questions referring to how well the scenarios helped the student reinforce course objectives, get feedback regarding their performance, and have an overall valuable learning experience. Nearly all (95%) participants perceived the patient simulator experiences as being valuable.
The individual items (7 items) related to the patient simulation experience were also evaluated (see Table 2). Sixteen of the seventeen participants felt the scenario adequately tested technical skills and prepared them for a testing experience. All respondents felt that to some extent the experiences adequately tested clinical decision making. More than 90% responded they were prepared for the testing experience. All participants felt the technical skills and decision making skills were valuable, but many participants (31.3%) expressed a need for an orientation before working with the patient simulator. Finally, some participants (23.5%) perceived the pace of the clinical simulation did not reflect the flow of an actual clinical setting.
Summary and Recommendations
Overall, these nursing students found the experience enhanced their learning and helped improve their decision making skills. On the whole, respondents were very positive regarding the transferability, realism and value of the patient simulation experience. However, the realism in regards to pace of the simulator experience could be improved by finding a way to demonstrate the passage of time found in the hospital setting. Also the value could be increased by providing more feedback to students regarding their performance with the patient simulator.
The limitations of this study are the small sample size and the lack of psychometric testing of the instrument. This small sample, 17 out of 48 eligible participants may give a misrepresentation of the perceptions of all students. The results of this pilot study will be incorporated into a larger study over a 2-year period involving simulation education through out the nursing curriculum. With a larger sample size, further psychometric testing through factor analysis will be completed and will determine the direction for strengthening the instrument.
The use of patient simulators in nursing education is an exciting and valuable method that appears to benefit students in their decision making skills, technical skills, confidence levels, preparation for “real-life” settings, and in reinforcing the learning occurring in class.
References
- Bearnson, C. S. & Wiker, K. M. (2005). Human patient simulators: A new face in baccalaureate nursing education at Brigham Young University. Journal of Nursing Education. 44(9), 421-425.
- Feingold, C. E., Calaluce, M.,& Kallen, M. A. (2004). Computerized patient model and simulated clinical experiences: Evaluation with baccalaureate nursing students. Journal of Nursing Education. 43(4), 156-163.
- Haskvitz, L. M. & Koop, E. C. (2004). Students struggling in clinical? A new role for the patient simulator. Journal of Nursing Education. 43(4), 181- 184.
- McCartney, P. (2005). Human patient simulators in maternal-child nursing. MCN. May/June, 215.
- Nehring, W. M., Ellis, W. E., & Lashley, F. R. (2001). Human patient simulators in nursing education: An overview. Simulation & Gaming. 32, 194-204.
- Nehring, W. M., & Lashley, F. R. (2005). Current use and opinions regarding human patient simulators in nursing education: An international survey. Nursing Education Perspectives. 25(5), 244-248.
- Nehring, W. M., & Lashley, F. R. (2004). Using of the patient simulator in nursing education. Annual Review of Nursing Education. l2, 163-181.
- Peteani, L.S. (2004). Enhancing clinical practice and education with high-fidelity human patient simulators. Nurse Educator. 29(1), 25-30.
- Ravert, P. (2002). Computer-based simulation in the education process: An integrative review. CIN: Computers, Informatics, Nursing 20(5), 203-208.
- Spunt, D., Foster, D., Adams, K. (2004). Mock code: A clinical simulation model. Nurse Educator. 29(5), 192-194.