Jared Peterson and Scott Steffensen, Department of Psychology
Introduction
Restless Legs Syndrome (RLS) is characterized by strong and often unpleasant urges to move ones legs while at rest and affects approximately 10% of the U.S. population1. The exact cause of RLS is not known, and the mechanism by which the urges are generated is poorly understood. One theory proposes that decreased oxygenation of tissues caused by increased levels of vasoconstricting cytokines may be the cause of these urges. The purpose of this project was to investigate the role that blood dopamine (DA) plays in this mechanism.
Past studies done in Drs. Steffensen’s and Mitchell’s labs at BYU have shown that patients with RLS have increased levels of DA in the blood compared to controls. Additionally, they have shown that RLS patients have close to half the percentage of lymphocytes expressing DA type 2 receptors (D2Rs) as compared to controls. Past research also reveals that DA has various immunological effects when it binds to these receptors, including the secretion of cytokines from immune cells2. Thus, our original goal was to show that increasing concentrations of blood DA cause a change in levels of secretion of vasoconstricting cytokines. However, because current literature maintains that only lymphocytes express D2R, we were surprised to find after initial trials that monocytes also express D2R. This novel finding led us to change our plan for this project. After careful consideration, we decided to further investigate how DA affects D2R expression on lymphocytes and monocytes in order to better understand the how each type of immune cell responds to DA before examining DA’s effect on cytokine secretion.
Methodology
To accomplish the above objective, we isolated white blood cells (WBCs), including lymphocytes and monocytes, from rat whole blood using lymphocyte separation media followed by red blood cell lysis according to a standard protocol. The white blood cells were then incubated with varying concentrations of DA for varying amounts of time. Control trials without DA and controls containing epinephrine or other agents were also performed. After incubation, cells were stained with antibodies that bind to D2Rs in accordance with typical staining protocols. Samples were then processed using Flow Cytometry to determine D2R expression.
Additionally, to better understand baseline D2R expression on monocytes of patients with RLS compared to controls, we used blood from RLS patients and healthy controls. Similar to above, we separated WBCs from whole blood, stained for D2Rs (without a DA incubation step), and processed the samples with Flow Cytometry.
Results
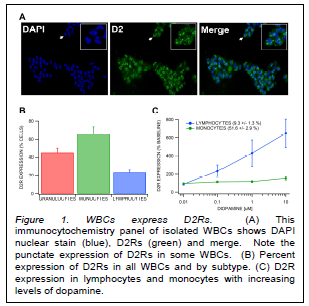
Our results indicated that not only do monocytes express D2Rs, but that they express them to a greater degree than do lymphocytes (Fig. 1, B). Additionally, we found that D2R expression in lymphocytes increases dramatically with increasing concentrations of DA, while D2R expression in monocytes remains mostly unchanged (Fig. 1, C). Lastly, the results of our RLS trials indicate that lymphocyte expression of D2Rs in patients with RLS is less than that of controls, while levels of D2R expression in monocytes are about the same between the two groups (data not shown).
Discussion
Our results are novel in that they are the first that we know of to positively identify D2Rs on monocytes. Interestingly, monocyte D2R expression does not seem to be a factor in mechanism of RLS given that RLS and control populations had approximately the same levels of expression. On the other hand, lymphocytes could play a more important role due to differences in D2R expression between RLS and control groups and that D2R expression was significantly altered with increasing DA concentrations. More research is needed to better understand the exact mechanism by which DA is influencing lymphocyte D2R expression.
Conclusion
With these experiments complete, we now turn our attention to the original question of this project: how does DA affect cytokine release? We regret that this aim of the project has been delayed, but we are excited about the opportunity to address that question now. The next phase of this project will hopefully help us understand how DA influences cytokines and how those cytokines affect patients with RLS.
