Daniel Sands and Erin Bigler, Department of Psychology
Introduction
Americans suffer an estimated 3.2 million concussions per year. Concussions are known to cause notable and long-lasting deficits in cognitive functioning in some individuals. This creates the need for new assessment tools and technology to facilitate assessment and treatment. This study will advance research in the use of functional Magnetic Resonance Imaging (fMRI) as an assessment tool in clinical neuropsychology. In recent years, cognitive tests have been adapted for administration in an MRI environment to enhance patient evaluation. However, meaningful interpretation of these test results requires normative data of healthy persons for individual patient comparison. In this project, we develop a normative database collected from a healthy population using six fMRI-compatible cognitive assessment protocols. We further demonstrate practical diagnostic application of this assessment model by presenting contrastive data from a collection of concussion patients. Upon analysis, patterns across concussion patients differed significantly from healthy controls, permitting an identification of five diagnostic neuromarkers for concussion.
Methods
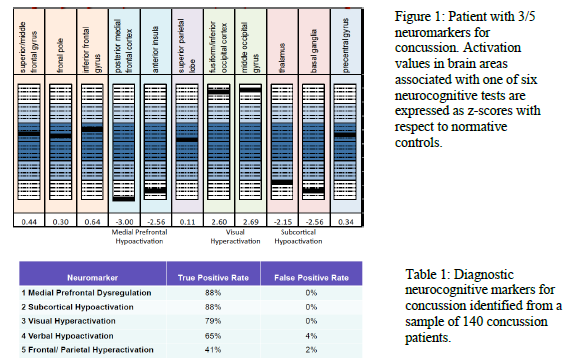
In 2012, Allen & Fong, co-authors with Dr. Bigler on a number of publications, recruited and scanned 51 healthy individuals who were currently not taking medications and had no significant psychiatric history. They used standardized protocols of six traditional neurocognitive tests adapted for fMRI use to track brain activity [blood-oxygen-level dependent (BOLD) signal] in 57 functional anatomical regions as participants performed cognitive tasks. The collected data was then analyzed to generate a standard of what a healthy brain should look like during each cognitive task. This allows individual concussion patients to be compared with the normative set to locate and quantify deficits in brain activation (see Figure 1). Allen and Fong then collected data from 140 concussion patients.
Using these archived and de-identified data, we compared both sets to distinguish deficit patterns in a concussed brain. Applying similar analysis methods used to generate the normative data, we compared each individual, both holistically and by brain regions of interest, against the concussion group and against the control group through multilevel t-tests and analyses of covariance. We examined patterns across concussion patients that significantly differed from those of the control group to identify possible diagnostic neuromarkers for concussion.
Results
Activation patterns across concussion patients differed significantly from healthy controls. Upon further analysis, we identified five diagnostic neuromarkers for concussion:
- Medial Prefrontal Dysregulation – Highly variable activation in attentional systems
- Subcortical Hypoactivation – Significantly decreased activation in areas of processing speed, visual tracking, and coordinated motor functioning
- Visual Hyperactivation – Significantly increased activation in areas of visual processing
- Verbal Hypoactivation – Significantly decreased activation in areas of receptive and expressive language abilities
- Frontal/Parietal Hyperactivation – Significant overactivation in areas of executive functioning We calculated the diagnostic power of each neuromarker by finding the true positive and false positive rates of each (see Table 1).
Discussion
Traditionally, clinicians have been limited to subjective symptom reporting to gauge and track concussion rehabilitation. Because fMRI provides a method that permits a more direct assessment of how brain activation relates to cognition, comparing individual patients against normative data will allow clinicians to objectively identify the specific underlying nature of a patient’s cognitive deficits. This could lead to the development of new and effective treatments for concussion in the future.
Conclusion
We demonstrate a standardized quantitative-fMRI model that is currently used for general neurocognitive assessment and treatment at the individual patient level, with a particular strength in concussion rehabilitation. Standardized administration of the proposed protocol in conjunction with both normative-based assessment and compliance monitoring for objective interpretation provides three elements which contribute to the establishment of practice standards for the clinical application of fMRI in guiding both neurocognitive assessment and treatment.